25 July in Victoria
Key points from Victorian Premier Daniel Andrews and Chief Health Officer Brett Sutton's latest coronavirus update
https://www.msn.com/en-au/news/australia/key-points-from-victorian-premier-daniel-andrews-and-chief-health-officer-brett-sutton-s-latest-coronavirus-update/ar-BB17avoo?ocid=msedgntp
Serco stands down Melbourne call-centre staff without pay on one day's notice
<<fears of new clusters in call centres full of casual and parttime staff who have minimal working conditions and no right to demand improvements in OHS settings to make their workplaces covidsafe>>
Melbourne hospitals braces for potential doubling in COVID-19 caseload next week
Mask wearing in Victoria is 'essentially Stage (Level) 4'
Victorian police crack down on rule flouting
'Stressing me out beyond belief': Government clarifies advice on maternity visits
More Victorians taking up ocean swimming during lockdown
Key points from Victorian Premier Daniel Andrews and Chief Health Officer Brett Sutton's latest coronavirus update
https://www.abc.net.au/news/2020-07-25/victoria-coronavirus-latest-cases/12491948Victorian Premier Daniel Andrews has described the state's second wave of coronavirus as "incredibly stubborn" as he revealed 313 health workers and one ADF member are considered active cases.
While giving his latest update on the situation, Mr Andrews said the state's aged care facilities remain "really challenging" environments because of a high number of casual staff and residents being older and vulnerable.
Meanwhile, the state's Chief Medical Officer Brett Sutton said increasing restrictions may not lead to fewer cases.
Here are some of the other key points from the update on Saturday afternoon.
https://www.abc.net.au/news/2020-07-25/coronavirus-australia-live-news-covid-19-blog-5-deaths-victoria/12491572What are the latest figures?
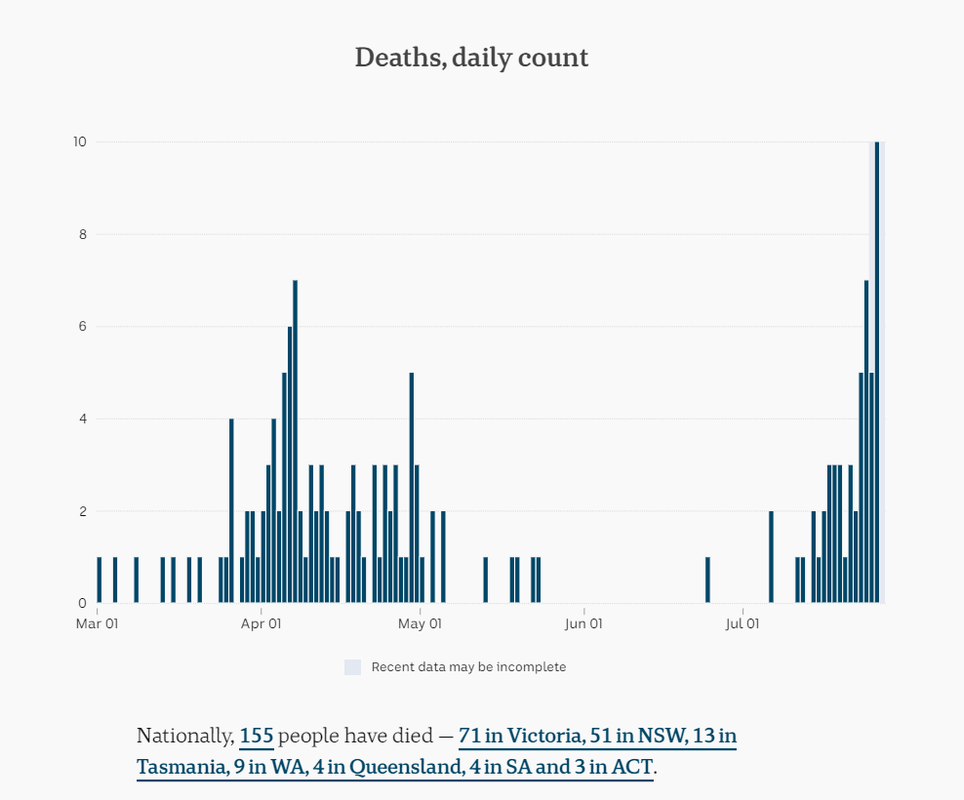
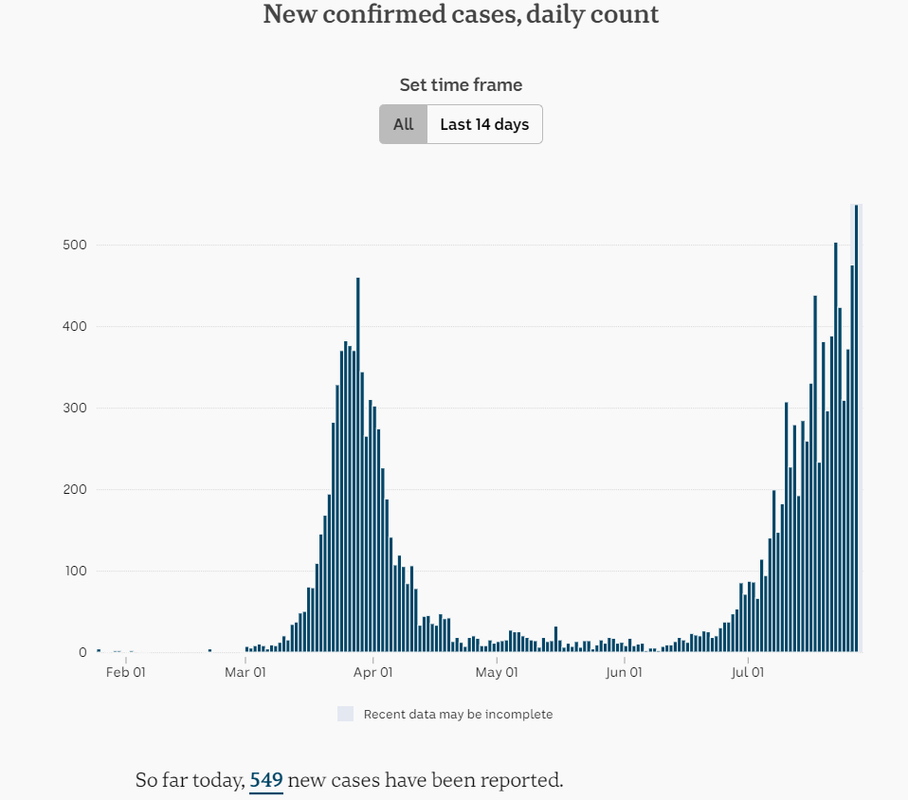
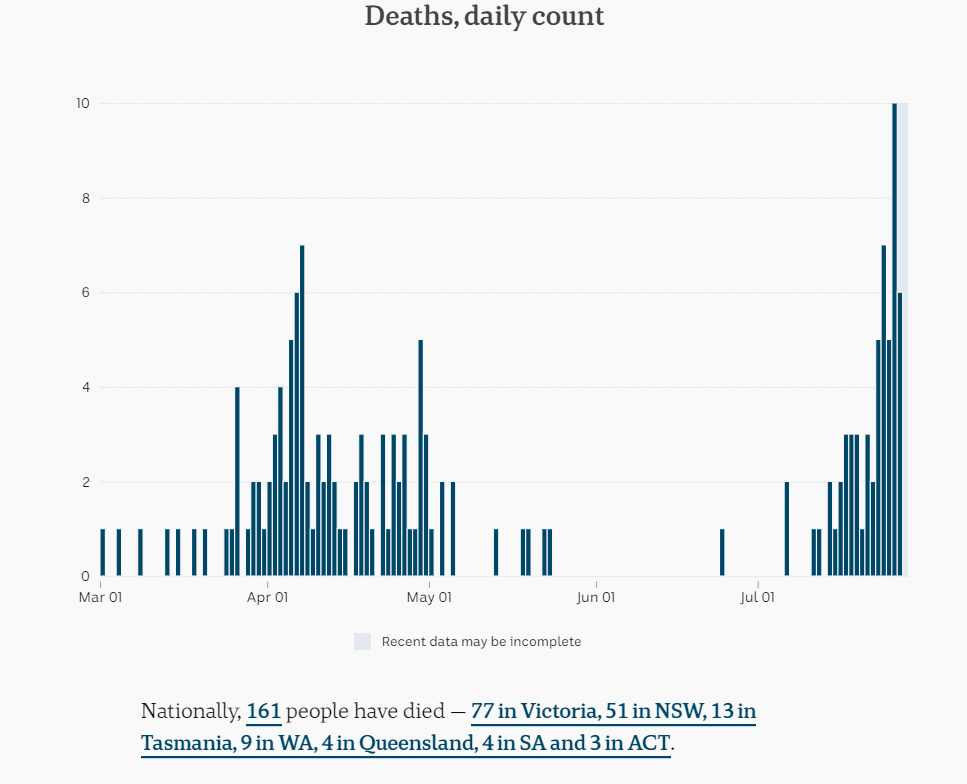
Victoria has recorded 357 new infections overnight including five more deaths.
The Premier said there were 3,995 active cases:
including 313 health workers,
one member of the Australian Defence Force
and 536 in aged care facilities.
The latest cases are linked to a number of outbreaks in Metropolitan Melbourne and regional Victoria, including an additional case linked to St Basil's Home for the Aged and three more linked to Estia Health in Ardeer:Victoria's coronavirus cases rise to 7,744 as five more people die from COVID-19Premier Daniel Andrews said a woman in her 60s, a woman in 70s, a woman in her 80s, a woman in her 90s, and a man in his 80s are the latest deaths, taking the state's death toll to 61.
There are 229 people in hospital, including 42 people in intensive care.
HOSPITALISATIONS BY AGE (AS AT JULY 24):
* 2 people aged between five and 19
* 5 people aged between 20 and 29, 1 in ICU
* 7 people aged between 30 and 39, 4 in ICU
* 11 people aged between 40 and 49, 4 in ICU
*14 people aged between 50 and 59, 10 in ICU
* 19 people aged between 60 and 69, 13 in ICU
* 30 people aged between 70 and 79, 7 in ICU
* 55 people aged between 80 and 89, 2 in ICU
* 22 people are 90 and aboveAsymptomatic Victorians who presented for a coronavirus test on Friday after having close contact with a confirmed infection told The Age they were turned away because they had not been approached by contact tracers.
New directives from the Department of Health and Human Services mean health workers at testing sites can only test asymptomatic residents who present a DHHS letter or text message.
'The following people are not currently eligible for asymptomatic testing: People living in previously identified 'hotspot suburbs' [and] people with letters from their employer, school or community group advising them to get tested,' the new DHHS guidelines state.
https://www.msn.com/en-au/news/australia/teetering-on-the-brink-of-catastrophe-coronavirus-cases-soar/ar-BB179GDj?ocid=msedgntp
Of the almost 4,000 active cases across Victoria, 313 are in healthcare workers.
There are also 536 active cases in aged care across 38 facilities, with roughly 50 per cent of them being residents and 50 per cent staff.
Mr Andrews said Victoria would be out of lockdown "as soon as we possibly can".
"I can't predict what tomorrow's numbers will be like, or where we will be in a week, let alone towards the middle of next month," he said.
"We will get out of this quicker than we otherwise would if everyone just stays the course, doesn't let their frustration get the better of them, follows the rules, keeps doing the magnificent stuff that so many Victorians are doing, wearing masks, staying at home, understanding that this is something that we all have to deal with."
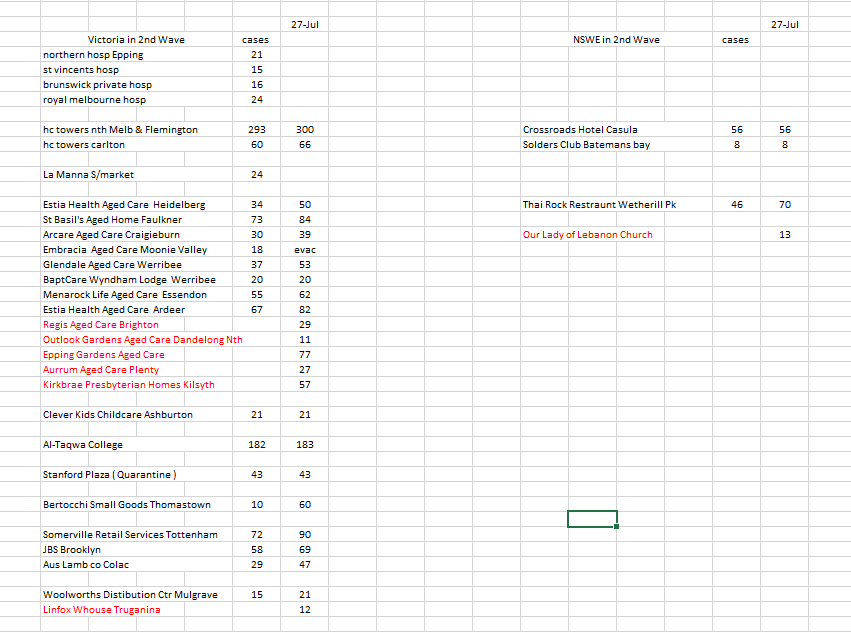
• 183 cases linked to Al Taqwa College
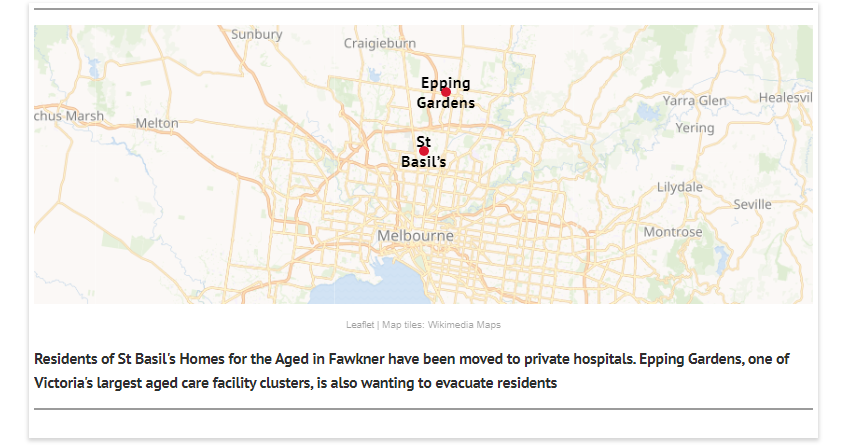
• 74 cases linked to St Basil's Home for the Aged in Fawkner
• 71 cases linked to Estia Health in Ardeer
• 60 cases linked to Menarock Life aged care in Essendon
• 44 cases linked to Estia Health in Heidelberg
• 49 cases linked to Glendale aged care in Werribee
• 23 cases linked to Baptcare Wyndham Lodge in Werribee
• 22 cases linked to Regis Aged Care in Brighton
• 80 cases linked to Somerville Retail Services in Tottenham
• 45 cases now linked to the Australian Lamb Company in Colac
• 21 cases linked to a Woolworths distribution centre in Mulgrave
• 10 cases linked to Star Track parcel distribution in Laverton
* 11 cases linked to Respite Services Australia in Moonee Ponds
* 9 cases linked to AMSSA in North Melbourne
* 6 cases linked to the Malmsbury Youth Justice Centre
* 5 cases have been liked to Steel Mains, a steel fabrication business in Somerton
* 4 cases have been linked to Waste Equipment & HIAB Services in Ardeer.
* 3 cases linked Diamond Valley Pork in Laverton North
* 3 cases linked to Sims Metal Management in Brooklyn
* 2 cases linked to Don KR Castlemaine
https://www.msn.com/en-au/news/australia/teetering-on-the-brink-of-catastrophe-coronavirus-cases-soar/ar-BB179GDj?ocid=msedgntp
Aged care with casual workers is 'really challenging'
There are more than 500 active COVID-19 cases in aged care centres, including 38 aged care settings.
Mr Andrews said it was roughly a 50-50 split of cases between health workers and residents.
He said the State Government is working in partnership with the Commonwealth Government and the private sector to put in place measures to curb the virus in aged care facilities, which has been largely driven by staff bringing the virus to work.
Mr Andrews said aged care centres were "really challenging" because they were staffed by many casual workers."We see that both in terms of the number of cases and also the number of people who are by the very nature of these settings frail and aged, many have underlying health issues," Mr Andrews said.
Measures put in place include:
Aged care settings 'very, very challenging'
Mr Andrews said aged care was a "very, very challenging environment" when it came to stopping the spread of the virus.
He said the Government was "working very closely" with the Federal Government and aged care providers to consolidate staff shifts into single sites to prevent "chains of transmission" being driven by staff.
"That obviously doesn't eliminate, but significantly reduces, the risk of the virus being transmitted by staff from one setting to another," he said.
"It is incredibly difficult to keep this out of aged care settings, particularly with such a transient and flexible and often insecure workforce."
Victoria's Covid-19 aged care disaster: 'this virus is like a fire out of control'
https://www.msn.com/en-au/news/australia/victoria-s-covid-19-aged-care-disaster-this-virus-is-like-a-fire-out-of-control/ar-BB179N5L?ocid=msedgntpThe disaster unfolding in Victoria’s aged care homes was “absolutely foreseeable”, one of the country’s foremost experts in aged care says.
Authorities knew some facilities had poorly trained workers and underpaid part-time or casual staff who had to move between homes to make a living. There’d been overwhelming evidence about the vulnerability of aged care residents internationally. In Sydney, there was the outbreak of Covid-19 at Newmarch House. It was all documented.
“We got this wrong from the very start,” says Prof Joseph Ibrahim, the head of the health law and ageing research unit at Monash University. The result, he and other experts say, is what is unfolding in Victoria.
The vast majority of aged care homes in Australia are privately-run and regulated by the federal government. There are now dozens of facilities with multiple cases. In total, there were almost 450 cases on Thursday across some 35 sites.
How did this happen? In early April, after Covid-19 had ripped through the Dorothy Henderson Lodge Aged Care home in Sydney, the regulator of aged care facilities decided to assess how prepared the country’s other providers were for an outbreak. They launched an online survey asking all facilities to declare if they were ready.
Of the 2,638 residential homes that responded, 99.5% told the Aged Care Quality and Safety Commission that they were ( ready )
<< yet no one checked by carrying out random unscheduled spot checks and inspection to confirm , Victoria's aged citisens are now paying the price >>
That was reassuring, but it was nonsense, says Ibrahim. The survey was about as useful as a police officer coming up to ask you if you were doing anything wrong.
“The survey was nice to do but asking people questions that they’re not aware of and not capable of answering and you’re the regulator [means] it’s not going to be a hand-on-heart moment, we’re in trouble, please visit us and give us a sanction.”
The critical government failure, says Ibrahim, was that while in the early days of the pandemic the focus was on a perceived shortage of acute care beds, ventilators and personal protective equipment, there was little obvious focus on aged care.
“In March, we had all of the stuff come out in Italy, Spain, France, England and the start of New York, all of that information told us that older people died far more in terms of fatality rates, and the highest fatality rate was for aged care or long-term residents”.
One report found that between 42% and 57% of deaths from the virus in various European countries were happening in care homes. The estimate is that, so far, about a 1/3 of fatalities in Australia are linked to aged care. In Canada, it’s 85%.For residents and their families, Melbourne’s outbreak is “terrifying”.
Ibrahim says the aged care outbreaks were predictable and state and federal governments are now playing catchup.
The wearing of face masks for all aged care workers was only made law on 13 July and then only in the locked-down Melbourne and Mitchell shire areas.
The interim report of the Royal Commission into Aged Care released in October 2019 laid bare the systemic problems in the sector – they were all known before the pandemic. A recent report found about 20% of facilities did not meet standards in “safe and effective personal and clinical care”.
<< Shelved and ignored when the sector cried "poor" and claimed was unable to implement recommendations because too expensive .>>
About 70% of the aged care workforce are personal care workers, often with a six-week certificate course as their qualification, with scant knowledge about deadly infection control. It is known that trained nurses have been a declining percentage of the workforce. A large percentage of the workforce are casuals or part-time workers, needing to work at multiple locations to make ends meet.
The Health Workers Union says 55% of their members in aged care work part-time, and 5% are casuals. Aged care workers often receive about $22 an hour, says union secretary Diana Asmar, and stopping them working a second job would drive many into poverty. The federal government, concerned about workers spreading the virus, is expected to announce a ban on working at multiple facilities next week.
With staff falling ill, there is a concern there won’t be enough workers in aged care facilities. The government has provided $234.9m for a retention bonus for workers in aged care facilities and in-home care, although the union says it should be provided for all workers including cleaners, kitchen staff and receptionists, not just carers and nurses.
The union, like Ibrahim, claims these problems have been known for years.
“If the aged care system was not working under usual circumstances, why on earth would anyone think that it would be able to ratchet up to perform extraordinarily well with this new threat?” Ibrahim says.
He argues the government should have months ago announced that every aged care home in the country would be case managed. The response has been too reactive.
Neither the state nor the federal government supports automatically transferring Covid-19 positive residents to hospital – instead saying it needs to be done on a case-by-case basis. The only state to enforce blanket hospitalisation so far is South Australia.
The Federal and Victorian governments will establish a response centre to coordinate efforts to curb the worsening situation in aged care facilities across the state.
The new centre will be jointly managed by Emergency Management Australia, Emergency Management Victoria and VicHealth.
Federal Health Minister Greg Hunt said it would be located at the Victorian State Control Centre and draw together the Australian Defence Force (ADF), Federal and State governments, the Aged Care Quality and Safety Commissioner, clinical leaders, geriatric support and emergency management.
"Its tasks will include quality control workforce provisions, prevention of outbreaks, rapid response, supporting provider communications to families and others," Mr Hunt said.
Workers consolidating shifts to a single site instead of working in many places, to reduce the risk of spreading the virus
The Commonwealth providing financial support to workers who are disadvantaged because they can only work in one place
The State Government paying $1,500 for a person in insecure work that tests positive and $300 a day when a worker gets tested and is waiting for their result
Reduced visitor numbers
Asymptomatic testing for staff
Additional training in infection control
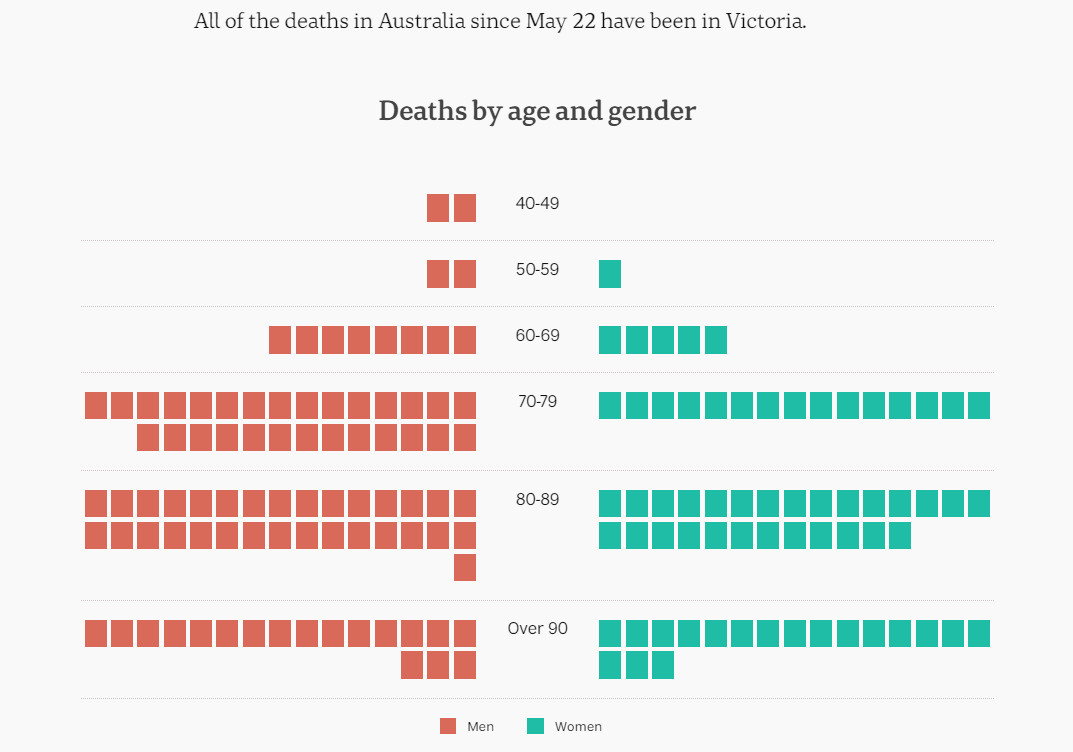
Victorian Chief Health Officer Professor Brett Sutton said the average age of residents in aged care is close to 90 years old.
"The severity of illness in that population is very significant," Professor Sutton said.
"Coronavirus is a very serious infection to get. The key is not having the virus introduced in the first place. Once you have an outbreak, their vulnerability puts them in danger."
Medically trained are getting sick
Professor Sutton said the case was being investigated.Professor Sutton said Saturday's figures indicated "a really challenging epidemic curve to overcome".
"I am hopeful and really keen to see what the effects of universal mask-wearing might be," Professor Sutton said.
He said treating the 229 people in hospital with the virus was a challenge but "relatively manageable".
"At some point, we will see a stabilisation in the active number of cases in Victoria, if our new cases remain stable. But it will continue to increase in terms of the admissions in acute settings for a couple of weeks after that," he said.
An Australian Defence Force officer who was supporting testing in Craigieburn has also tested positive to the virus.
Professor Sutton said it was not clear how the ADF member caught the virus and it would be investigated.
He said the case highlighted how infectious the disease was, when an ADF staffer who was medically trained and wearing personal protection equipment (PPE) tested positive.
"Even those medically trained individuals using PPE and who have been trained in it and have been given all the appropriate PPE, can be at risk," he said.
"Sometimes it is in the donning or the doffing, or the washing of hands before and afterwards … It speaks to the absolute infectiousness of this virus."
Mr Andrews said he was grateful for the work of the ADF.
"Even with the full PPE, layer upon layer, no PPE can reduce the risk to zero. But ADF are playing a really important part, and we are very grateful to them, " he said.
Why stage 4 restrictions won't help?
Professor Sutton says this wave of infection is "not like the first wave".
"The numbers have remained stubbornly high," he said.
This week, people in Melbourne and the Mitchell Shire must don a face mask when outside their homes, the latest measure to reduce infections.
"I am hopeful and really keen to see what the effects of universal mask wearing might be," he said.
Many people are speculating the State Government may need to tighten restrictions, but Professor Sutton says the focus remains on preventing transmission in aged care centres and workplaces like warehouse distribution centres and food production facilities.
"The very places where we are seeing outbreaks, the very places where we are seeing transmission, are the places that would remain open if we went to a stage four," he said.
"We shouldn't pretend that a really broad shutdown of industry will address where we are seeing the transmission."
Beware of scammers
People are being warned to be on the lookout for scammers wanting bank details.
The Australian Competition and Consumer Commission (ACCC) states its Scamwatch program has received 3,550 scam reports mentioning the coronavirus.
The Premier said reports of scammers posing as officials were "an ugly feature of our modern world" and "awful".
"No member of the contact tracing team is going to be asking for your credit card or your bank details," he said.
He did note if you have claimed the Government's $300 or $1,500 payment, you will be asked for those details.
Mr Andrews said he was confident that between the Health Department, Consumer Affairs Victoria and potentially police, the matters would be investigated.
Army move into Colac to help contain spread from abattoirMeanwhile, the Australian Defence Force has arrived in Colac in Victoria's south-west to help with contact tracing efforts.
The number of active coronavirus cases in the town jumped from zero to 45 in just over a week after an outbreak at the Australian Lamb Company.
The abattoir is the town's largest employer with about 700 employees.
An incident control centre has been set up in the regional town to support contact tracing, testing and to ensure the community receives information about the evolving situation.
Three ADF members are helping with logistics, and up to 20 are expected to arrive on Monday to support a re-testing blitz.
Mark Gunning, from the Country Fire Authority, is part of the incident control team and says it will also provide food, relief packages and health support to those in quarantine.
"The idea of the [incident control] team is to bring all those parties together, to work collaboratively, so there's not ambiguity in messaging," he said.
"[Then] people can be really clear on what they need to be doing to stay safe."
ADF members will consist primarily of medical staff and be supported by general soldiers.
Mr Gunning said more people in the community were wearing masks, adding that it was vital everyone socially distanced and maintained good hygiene.
"Please, if there's a reason why you've got a test, if you've got symptoms or you've had a close contact, if you get a test go home, stay home," he said.
https://www.msn.com/en-au/news/australia/key-points-from-victorian-premier-daniel-andrews-and-chief-health-officer-brett-sutton-s-latest-coronavirus-update/ar-BB17avoo?ocid=msedgntp
Serco stands down Melbourne call-centre staff without pay on one day's notice
<<fears of new clusters in call centres full of casual and parttime staff who have minimal working conditions and no right to demand improvements in OHS settings to make their workplaces covidsafe>>
https://www.msn.com/en-au/news/australia/serco-stands-down-melbourne-call-centre-staff-without-pay-on-one-day-s-notice/ar-BB178dp8?ocid=msedgntpMultinational outsourcing giant Serco gave staff at a Melbourne call centre just 24 hours’ notice before standing them down without pay indefinitely because of a Covid-19 outbreak, after they had spent months helping Australia’s surging numbers of unemployed.
The outbreak forced the closure on Monday of the Mill Park call centre in Melbourne, which helps fulfil the company’s Centrelink call centre contract with Services Australia.
Documents obtained by the Guardian show Serco has stood down all of its workers indefinitely.
The company wrote to staff on Wednesday telling them they would be stood down without pay from Thursday.
“The stoppage of work means that you are now stood down from work in accordance with section 524 of the Fair Work Act 2009,” Serco’s contract manager, June Meldrum, said in the letter.
“You will receive your ordinary pay in accordance with any confirmed shifts for today. For full time or part time staff, unpaid stand down will commence from Thursday 23 July 2020 onward. These people may, however, elect to utilise their annual leave entitlements during this period.
“Casual staff will not be rostered from Thursday 23 July 2020 until further notice.”
No mention was made of working from home, though the company has said it is attempting to work with its government client to institute such arrangements.
The letter told staff they remained “valued” by Serco.
“I confirm that while you are stood down, you remain a valued employee of Serco. However, we of course understand that you may need to make other arrangements during this period.”
A Serco spokesman said the company was working as hard as it could to have staff back performing essential government services “as soon as possible”.
“This is obviously an extremely difficult time for our Mill Park team, and we are doing all we can to safeguard our employees’ health and safety following the directive given to us by [the Department of Health and Human Services],” the spokesman said.
One source suggested to the Guardian that staff had continued to hot-desk throughout the pandemic, posing an unnecessary risk.
The company denied that claim. It also stridently denied any suggestion that the six cases it had recorded among call centre workers in July had been a result of staff-to-staff transfer.
Related: Home affairs fought for three years to stop Serco detention centre manual release
A spokesman said Serco was conducting temperature checks of staff, had placed perspex screens in workstations, employed “full sanitation protocols”, offered face masks, and conducted deep cleans.
It closed the centre last weekend voluntarily but decided to keep it closed on advice from the DHHS.
Serco said the department deemed that all employees of the call centre were “close contacts” of known cases, meaning they were required to self-isolate for the quarantine period and be tested.
Services Australia said the closure of the call centre would not affect its services.
It described the Serco closure as “precautionary”.
“Our services are not affected as Services Australia’s call centre network spans across the nation, including thousands of additional staff taking calls and processing claims as part of our coronavirus response,” the department said in a statement.
“Serco took a precautionary step to immediately close the Mill Park site and will work with the Victoria government’s Department of Health and Human Services to ensure the workplace is safe before reopening.”
The department also said it required all contractors to strictly adhere to the health authority requirements of the relevant states and territories.
Melbourne hospitals braces for potential doubling in COVID-19 caseload next week
https://www.msn.com/en-au/news/australia/melbourne-hospitals-braces-for-potential-doubling-in-covid-19-caseload-next-week/ar-BB17ahp0?ocid=msedgntpMelbourne hospitals are bracing for a surge in coronavirus patients after confidential modelling by the city's major hospitals suggested cases could almost double over the next five days.
Yesterday, seven deaths and more than 300 cases were recorded in Victoria in what was the state's deadliest day.
The situation at aged care facilities continues to spiral out of control with five of those deaths and more than 200 infections aged care residents.
Aged care in Victoria is looming as a coronavirus disaster — brace for it to get worse
https://www.abc.net.au/news/2020-07-25/coronavirus-aged-care-deaths-victoria/12491538Brace for it to get far worse from here.
In the past fortnight, 34 Victorians have died with COVID-19, more than doubling the state's death toll from the virus.
But aged care stands as a looming disaster for the state, after a dramatic growth in infections across a growing list of nursing homes.
The total number of infected residents of nursing homes nationwide has quadrupled since the start of the month, from 71 to 292 and counting.
Almost the same number of nursing home staff have also been infected.
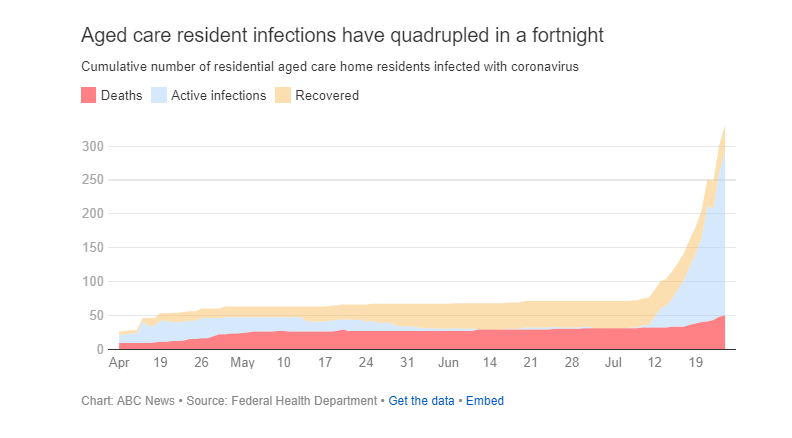
Residential aged care homes have been among the deadliest environments in this pandemic.
According to the Federal Government, at least 48 people living in residential aged care homes have died with COVID-19, as well as a further four people receiving in-home care services.
Before the current outbreaks in Victoria began, of the 71 aged care residents infected, 31 died and 40 recovered.
That is, 44 per cent of infected residents didn't survive, a horrific statistic.
As of Friday, there were 242 residents who were fighting the virus.
There's a strong likelihood the next few weeks will be grim.
We've seen this before
In the first wave of the pandemic, two serious nursing home outbreaks devastated Anglicare's Newmarch House and the Dorothy Henderson Lodge.
There were 71 infections among staff and residents at Newmarch House alone, and 17 deaths.
Later potential crises in aged care managed to be avoided, including at a nursing home in Rockhampton.
But now there are cases linked to at least 40 aged care homes in Victoria, and some of the outbreaks rival Newmarch House in size.
With many homes still curtailing family visits due to the threat of infection, the virus has typically been brought in by staff inadvertently.
The Aged Care Quality and Safety Commission is examining how nursing homes manage the crisis and has already taking compliance action, including against Menarock last week.
"The Commission took regulatory action in relation to Menarock Life Essendon Aged Care Services because of significant concerns about the provider's response to the outbreak and the safety, health and wellbeing of the residents at the service," commissioner Janet Anderson said last week.
"Menarock Life Aged Care Services has notified the Commission that it has accepted the requirements imposed by the Commission under the regulatory action."
The regulator has also taken regulatory action in relation to Newmarch House.
Mask wearing in Victoria is 'essentially Stage (Level) 4'
https://www.msn.com/en-au/news/australia/mask-wearing-in-victoria-is-essentially-stage-four/ar-BB17a5Rm?ocid=msedgdhp#image=1Mr Andrews said the wearing of masks is essentially the state in "stage four lockdown".
Health authorities now encouraging mask usehttps://www.msn.com/en-au/news/australia/health-authorities-now-encouraging-mask-use/vi-BB17a1S9?ocid=msedgntpNick Talley, Editor-in-Chief of the Medical Journal of Australia, says evidence now shows that masks help stop the spread of COVID-19.
"If they are worn by everybody then we may not need to go further," he said.
"We cannot rule out going further with rule changes, but it is a big game changer, potentially, and I cannot tell you how proud I was to travel in here this morning and see literally every single person on my journey into the office from the middle ring suburbs in the south-east, wearing a mask. It is just a fantastic thing.
"And while people were a bit concerned and that was a bit of talk back and forth about whether it would happen, it is happening, it makes you proud, it is a significant step we can all take to potentially slow and limit the spread of this virus and then drive down case numbers."
He said Victoria Police is "out there" and will fine people who don't wear masks and will take action against you.
"By following these rules, and getting to the other side of the second wave," Mr Andrews said.
Victoria's Chief Health Officer Dr Brett Sutton said the second wave is not like the first.
"The numbers have remained stubbornly high, haven't gone up significantly, haven't gone down significantly in the last week," Dr Sutton said.
He said if the state went to a formal stage four lockdown, the areas where there are significant outbreaks, such as aged care homes and schools, are the places which would remain open.
"So these are the areas we need to focus on, and we shouldn't pretend that a really broad shutdown of industry will address where we are seeing the transmission," Dr Sutton said.
"We need to really focus on how do you prevent transmission occurring in aged care, and the premier has listed some interventions we are working on there stop the spread for healthcare settings…food distribution centres, other warehouse distribution centres and food production facilities."
He said mask usage is essential to work towards stopping the spread and is hopeful of the results.
"But I do think, you know, the fact that we have got universal mask usage now, really, for the community, both going out of your home but also in all of the workplaces that people are attending, that is something that will address both these high risk settings, but also every other workplace," he said.
Mr Andrews said the current situation is a crisis, and he is working closely with the Federal Government to beat the outbreak, especially in aged care homes.
He said he is working closely with the Prime Minister for the "really challenging setting".
"We see that both in terms of the number of cases and also the number of people who are by the very nature of these settings frail and aged," Mr Andrews said.
"Many have underlying health issues. It is a very, very challenging environment, and I want to send my support and assurance to all families and staff, all of those involved in aged care, that many different steps have been taken, processes have been put in place."
He said state and federal governments, with the union, are looking at staff shifts and how the spread of the virus can be stopped.
Victorians urged to wear a mask while exercising
https://www.msn.com/en-au/news/australia/victorians-urged-to-wear-a-mask-while-exercising/ar-BB17asOf?ocid=msedgntpMelburnians doing exercise are being urged to wear a mask, despite being exempt from the new rules.
The state's Chief Health Officer Dr Brett Sutton said wearing a mask is "just a good idea all round", especially as people expel more air droplets, which could lead to the spread of coronavirus.
Rules this week came into place making face masks mandatory.
"We have made an exemption for people who are doing strenuous exercise, but I would say, if you can wear a mask when you are cycling, or when you are running, wear a mask, absolutely," Dr Sutton said.
"When you are exercising, you do breathe out more forcefully. But we have made consideration of the fact that for some people, doing strenuous exercise, they couldn't manage it with a mask on. So they needed that exemption.
"It doesn't mean that we wouldn't recommend a mask under normal circumstances, if they can manage it. But for some people, it makes breathing difficult.
"I am aware of people who can run a marathon in a mask. If you are one of those people, absolutely, wear a mask, running, cycling or anything else that is strenuous.
"But the exemption is there for the people who cannot manage that exercise otherwise."
Melburnians are allowed outside to exercise as one of the four reasons they can leave their homes.
Masks part of the Melbourne look for a long time to come
https://www.smh.com.au/national/masks-part-of-the-melbourne-look-for-a-long-time-to-come-20200715-p55c5i.htmlMelburnians may need to wear masks on public transport and in other busy public spaces until there is a widely available vaccine for coronavirus.
University of NSW epidemiologist Mary-Louise McLaws said wearing face masks would be a significant cultural shift for Victorians, but a necessary means of protection in the battle against COVID-19.
"Wearing face masks is something that should become a part of people's everyday lives until a vaccine is found or this virus stops being a threat," the World Health Organisation adviser said.
Until Victoria drives cases down to single digits for at least a fortnight, those living in Melbourne or the Mitchell Shire should not go out in public without their nose and mouth covered, Professor McLaws said.
Police in Melbourne have been told to wear masks while working in their stations, it emerged late on Wednesday.
"Victoria Police has recommended staff wear face masks within controlled Victoria Police workplaces where physical distancing cannot be maintained, including where no contact with the public occurs," members have been advised.
As debate mounted on whether the state could achieve elimination of the virus, Victoria's Chief Health Officer, Brett Sutton, said on Wednesday that mandatory mask-wearing "shouldn’t be off the table", but he warned against police punishing people who could not access a mask.
<< Cops are actually providing free surgical masks people who have not been able to afford or find masks for sale for reasonable prices ( yes the price gougers are active AGAIN , including shamefully chemist chains and local chemist shops , hardware shops and supermarkets ) with warnings in Victoria .>>
"It’s a risk not to have them, especially with the transmission going on in Melbourne," Professor Sutton said.
People entering Victorian courts and tribunals are now strongly encouraged to wear face masks with security staff handing out disposable versions.
Is the aim elimination ( extinction of ) Covid19 or suppression of community transmission to a defacto elimination scenario ( single figure cases per week statewide ).
Asked whether Victoria should switch to an elimination approach to the virus, Professor Sutton said: "I'd love elimination, but it's not the right time to be assessing whether that is feasible right now."
When pressed on the likelihood of a harsher stage four lockdown in Victoria, Professor Sutton said any potential hardening of restrictions would be targeted at areas creating the biggest problems.
"If we’re seeing a focus in a particular setting, in a particular cohort of people, related to particular activities, that would be the focus of stage four restrictions," he said.
Professor Bill Bowtell, of UNSW's Kirby Institue for infection and immunity said, however, that the suppression strategy in Victoria was failing and called for the adoption of an elimination strategy.
He also questioned why Victorians weren't encouraged to wear masks sooner when infections began to climb in March.
“Do we keep on putting people in lockdown or do we go for hard lockdown and aim for eradication, which can be done and has been done?” asked Professor Bowtell, who helped lead Australia's response to the AIDS crisis in the 1980s.
"New Zealand did it and they haven't had community transmission in 70 days. This is a virus, it's not a supernatural zombie. It transmits between people so you need to separate people."
Tony Blakely, a University of Melbourne epidemiologist, is also pushing for Victoria to move into a hard lockdown.
“We know from lots of international experience now, the best one being Wuhan, you can basically knock this virus out of the park if you decide to lock down hard," Professor Blakely said.
"Given that we’ve already gone into a lockdown in Melbourne, we should turn something that depresses us into an an opportunity. In the six weeks of hard lockdown we could actually achieve elimination."
For this to work, the "loose definition" of what essential workers are must be tightened and Victoria would mirror the "New Zealand prototype", Professor Blakely said.
Places such as abattoirs, which have battled multiple outbreaks, should close for at least a month, along with schools, educational facilities and every business except essential services such as supermarkets, pharmacies and medical clinics.
However, Dr Nick Coatsworth, the federal Deputy Chief Medical Officer, has warned that elimination would be a risky strategy.
"The risk elimination creates is a false sense of security that may diminish the community engagement with widespread testing and lead to a downsizing of the enhanced public health response, based on an assumption “we have got rid of the virus once and for all in our part of the world”.
University of Melbourne epidemiologist Professor John Mathews argued that it might be too soon to aim for zero.
"It is impossible to go for elimination without suppressing it first," he said. “At the moment, one couldn’t rule out the possibility that in a week or 10 days' time, we’ve got a disaster on our hands."
Griffith University infectious diseases expert Professor Nigel McMillan said even if the virus was eliminated, Australia must "still deal with the rest of the world in some manner".
"Elimination won’t be a golden answer to your economic woes, especially in a country like New Zealand or Australia that relies on tourism," he said.
Professor McMillan said for the state to avoid future outbreaks, Victorians would have to change their way of thinking and remain vigilant not only during the lockdown period, but for the months or even years ahead.
"There are probably quite a few people who have said 'it’s just one thing, it’s just a small get-together with my family,’ but of course it does matter. We’ve got to eliminate that sort of attitude," Professor McMillan said. "It only takes one or two people to not do the right thing and it’s away."
Victorian police crack down on rule flouting
https://www.msn.com/en-au/news/australia/victorian-police-crack-down-on-rule-flouting/ar-BB179dOy?ocid=msedgntpVictoria Police have warned they will crack down hard on any Victorian's flouting lockdown measures.
It comes as video emerged of a woman intentionally trying to cross a border checkpoint without giving a legitimate reason.
Over the past 24 hours the police have conducted 5,300 spot checks and dished out 101 fines and 63 warnings.
Police are now being assisted by the Australian Defence Force with contact tracing and door knocking procedures.
'Stressing me out beyond belief': Government clarifies advice on maternity visits
https://www.msn.com/en-au/news/melbourne/stressing-me-out-beyond-belief-government-clarifies-advice-on-maternity-visits/ar-BB176Vu7?ocid=msedgntpThe government has changed its advice to expectant mothers and clarified that there will be no limit on how long partners can remain with new mothers in the hours after they give birth.
Expectant parents were left confused and alarmed after the state government said on Thursday that as part of measures to stem the spread of COVID-19, partners or a support person could stay at the hospital for only two hours after new mothers were moved from the birthing suite to postnatal care.
"From today, the rules that apply to maternity situations is that the woman is able to have her partner or support person for as long as is required for the entire labour and birth of their newborn baby and then their partner or support person is able to be with them for a two-hour visit after the baby is born," Health Minister Jenny Mikakos said at a press conference on Thursday.
"This addresses some of the concerns we have seen in relation to at least one health service that I'm aware of in the last week. We have tried to strike the balance there between compassion and safety."
he position was confirmed by Ms Mikakos' department after the media conference with a statement saying that ''on the day of the birth, once the mother and newborn move to the postnatal ward, a partner or support person can stay for up to a further two hours.
''A partner or support person can then visit once per day for a maximum of two hours every subsequent day the mother is in hospital."
However, late on Thursday night, Ms Mikakos said partners can stay as long as required on the day of the birth, but visits on the days after the birth will be capped at two hours.
"The only thing that's changed is a pregnant woman giving birth can now have one visitor when before it was two," she wrote on Twitter just before 11pm on Thursday.
"Her partner/support person can stay for as long as they wish during labour and birth and after the baby is born."
Visiting restrictions will be tightened across Victorian hospitals and aged care facilities as case numbers continue to rise among healthcare workers, nursing home staff and residents.
Only one person can visit hospital patients and aged care home residents for one hour a day, but there will be exceptions for parents with children in hospital and visitors of patients in palliative care.
Other exceptions include nominated mental health supporters, people providing language support and people visiting patients in life-threatening situations.
"This addresses some of the concerns we have seen in relation to at least one health service I'm aware of in the past week," said Ms Mikakos on Thursday. "We ask for Victorians' understanding at this challenging time."
More Victorians taking up ocean swimming during lockdown
https://www.msn.com/en-au/news/australia/more-victorians-taking-up-ocean-swimming-during-lockdown/vi-BB17a3UD?ocid=msedgntpMany of the swimmers say cold water immersion has helped them deal with the stress of lockdown, and been a welcome distraction from the pandemic.
<< this is something along the lines of an immune system booster suggested a few times on MEDCram >>